In this particular blog I want to discuss my sons other early developments and how this can help facilitate the rehabilitation process.
Lets review some early developments and some integrated reflexes.
Month 1:
-Begins to lift head when on stomach (prone).
– Breathing (diaphragmatic)
– Begins to make cooing/gurgling noises.
– responds to stimuli/particularly sound and light
– Follows object with Eyes.
– Random and unintentional arm and leg movements.
– smiles and laughs -poor head control in vertical
-eye focus 8-12 inches from face.
Month 2:
-improved head lifting when prone (able to hold for short periods) – smoother and intentional arm and leg movements.
-some head control into flexion (moving head off surface when on back) (pulling baby off his back)
– begins to lift head and shoulders when prone (on elbows) – makes louder, more intentional sounds
– begins to grasp objects.
-begins to accept some weight when stood on legs.
-improving head control in vertical
-eyes focus 12-24 inches from face.
Month 3: – good smooth pursuit and visual tracking
TLR (tonic labyrinthine reflex): a primitive reflex found in newborn humans. With this reflex, tilting the head back while lying on the back causes the back to stiffen and even arch backwards, the legs to straighten, stiffen, and push together, the toes to point, the arms to bend at the elbows and wrists, and the hands to become fisted or the fingers to curl. The presence of this reflex beyond the newborn stage is also referred to as abnormal extension pattern or extensor tone.
ATNR: is a primitive reflex found in newborn humans, but normally vanishes around six months of age. When the face is turned to one side, the arm and leg on the side to which the face is turned extend and the arm and leg on the opposite side flex.
STNR: a primitive reflex found in newborns which links head movement to arm and leg movment. When the head extends, so do the arms, while the hips and knees flex. When the head flexes, so do the arms and shoulders and the legs extend.
We touched on breathing and how it primes the core. This provides the base of stability in which all our other movements occur. We could say that this drives our internal sense of stability. This anchors us to our self.But we also must anchor ourselves to the external world. Sometimes, especially in injury (particularly to the spine; even more to the neck) our internal calibration gets off and we seek to correct this from the outside world.
We use 3 systems to do this. The visual. The proprioceptive. And the vestibular. Today we will focus on the visual and some on the proprioceptive system in the neck. The other systems are already active and being processed but for our purposes lets take it one at a time.
Even before we jump into visual developments and their implications we must discuss a bit of light neuroanatomy.
Lets all take an understanding of one thing: the brain is in charge. Without it, we die. We are our brains. Without it our bodies cease to function. So when I say that dysfunctional movement is a result of the brain, it is because the brain integrates sensation and drives movement.
The brain is divided in half- left and right. Due to a serious and complex wiring job, the left half is responsible for the right half of our body and the right responsible for the left. (For the most part, as with everything there are exceptions). This is intentional. I read somewhere that ‘we are both wonderfully and fearfully made’. Our anatomy and body is clearly made for a purpose. Why our nerves cross is beyond the scope of this blog, but know it happens for a reason.
The two halves are divided into front and back.
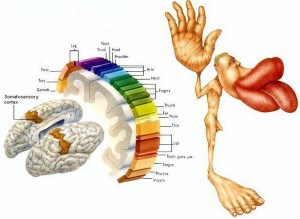
The back halves are responsible for interpreting the sensory information that we are presented in our daily lives: noise, touch, taste, sight, smell (also our joint position sense: proprioception) . This is our somatosensory cortex.
The front halves are responsible for our responses to this sensory information: it generates programs for movement to coordinate muscle firing and create intentional movement patterns. This is our motor and premotor cortex.
It must be noted at this point : sensory information drives our motor responses. Without quality sensory stimuli our motor responses will be altered. Sensory responses can be altered through thoughts, previous experiences, spinal cord injuy, brain injury, poor joint position or muscular length, sensation alteration, (read neuropathy due to diabetes anti -cancer drugs etc).
Note that the biggest parts are the areas with the most dense nerve endings. If we accept that sensation drives our motor performance, then these areas become increasingly important to utilize when in rehab.
Clearly one of the largest areas on the homoculus is the head and face. Not surprisingly, after (in reality, all these things happen simultaneously) baby learns to breathe, he starts to move his eyes, head, and neck. These areas are very important to the body because they house and protect our brain (the mothership) and are the center for the vast majority of our senses.
Once a stable core facilitated through breathing, my baby started to explore his world. This first happened with his eyes. As the milestones suggest visual acuity is limited in the beginning to about 8 inches. As deliberate as these things can be its been found this is highly correlated with the length of a baby’s arm. (More on this in a minute).
Lets talk eyes. Even before he was born, my son reacted to a light shown on my wife’s belly. And even more so after birth. This is a sensory stimulus driving a motor reaction. When Owen sees or hears something of interest to him he moves his eyes first towards that stimulus, followed by his head. Looking up facilitates neck extension, to the side rotation, and down neck flexion. This is important. Studies have shown that in a normal population, when prompted by a stimulus, the small muscles controlling the eyes fire first followed by the neck second. We look, then turn. In painful pr dysfunctional situations, it has been found that the eyes fire second and the neck fires first. This creates a situation in which the body expects a visual confirmation relative to neck position and gets a much different feedback because the neck moved first. This mismatch of expectations and actuality creates sensory conflict. Much like feeling like your car is rolling backwards when a car beside you drives forward the body reacts based upon he expectation of what the brain percieves is going on. This can cause visual disturbance, dizziness, vertigo, muscle spasms and more. And it leads to body to try and protect itself in the flexed position we discussed in the last blog. If the body doesn’t trust its eyes, it will attempt to limit head and neck motion by generating tension in the cervical muscilature to limit head movement and thus the need.for the eyes to move. When the eyes fail to report accurately, many impairments can result.
The eyes require a stable point of fixation. This means the head must sit on a stable cervical spine. This is accomplished through activayion of the deep cervical stabilizers, longus colli and longus capitus. We know this as the chin tuck maneuver. While often lost this day and age due to prolonged sitting, a neutral neck is important to allow the body a point from which it can say is neutral. Without this, the body is less certain where neutral postures are. As Owen learns and interacts he preps his body for movement with his diaphragm and his neck. Charlie Weingroff talks a lot about the importance of neck neutral and ‘packing the neck’ during exercise. Check this link out for more on the packed neck.
From a rehabilitation standpoint, we can utilize eye movements to generate predictable neck and body responses and improve neck range of motion and exercise response simply by tapping into the body’s natural tendency to follow the eyes. If we are interested in increasing the body’s ability to flex we can have the patient look down with their eyes. If we are interested in increasing extension, we can accent this by looking up. The same goes for all movements. We can accent intended movements with eye movements to help cement them in our body’s movement repertoire. Likewise, we can see certain movement patterns become less effective when eye movements contradict the intended patterns. Take a hip hinge which we use to help promote flexion. Or a dead lift which is the weighted progression of the hip hinge. We see many faulty lifts and body positions due to inability to maintain cervical position and use the eyes. Often with these movements we see patients bringing their head neck and eyes into full extension as the body lowers. This confuses the brain by combining a flexion based movement with extension based head and eye movement. It also takss the neck out of a stable ‘packed neck’ positon. When this happens we also must take into consideration that the patient is tapping into primative reflexes to accomplish movements. In this case we see the patient utilizing the STNR (head extended with relative lower extremity flexion) to get through the motions. Primitive reflexes, while important for development are needed to disappear for normal movement patterns to evolve. Use of primitive patterns to accomplish movement demonstrates significant challenge to the brain with movement processing. This is dangerous to continue to reproduce as the body learns to move using a regressed pattern. Some clinical presentations of this use of regressed patterns are patients with cerebral palsy or patients who have had a stroke and develop spasticity in a flexed or extended pattern.
As we can see, the hands are also a large and important part of our body. The input they provide in combination with other information begin to create a picture of the world to my son.
As I mentioned before, a baby’s arm happens to be near the perfect focal length for his eyes. This is not coincidence. The allows the baby to put his hands (sensory goldmine) and his eyes (jackpot!) To work together. This is valuable stuff. Lets revisit the ATNR where the head turns and the arm outstretched in front of it. Like this:
The link of the hands to the eyes links two very important body recognition systems – the visual and the proprioceptive. When sensory systems align the body recognizes this alignment and balance within the body and correlates with the diaphragm and neck and inner core stability to dial in and produce quality movement. This quality movement is efficient and preferred by the brain. This then, with repetiton becomes the preferred pattern of movement and how we, as humans, progress and improve motor control skills. From a rehab standpoint, we can accent and improve on the body’s natural patterns of movement to engage motor learning and skill acquisition.
From these first two blogs I’m attempting to define some baseline tenants of rehab from my standpoint:
1. A stable core unit must be established. This means proper diaphragm use and breathing and the ability to adopt and maintain a stable neck using the packed neck position.
2. We can and should use eye movements and even tongue movements to accent and enhance full body motions.
3. Quality sensory input and body position will drive and produce more effective movements. Using sensory dominant body parts cant help provide quality input.